PressureSafe: Universally-applicable assessment of pressure injuries
Home » Pressure Injury

Drivers for adoption of PressureSafe for assessment of Pressure Injuries before skin breakage
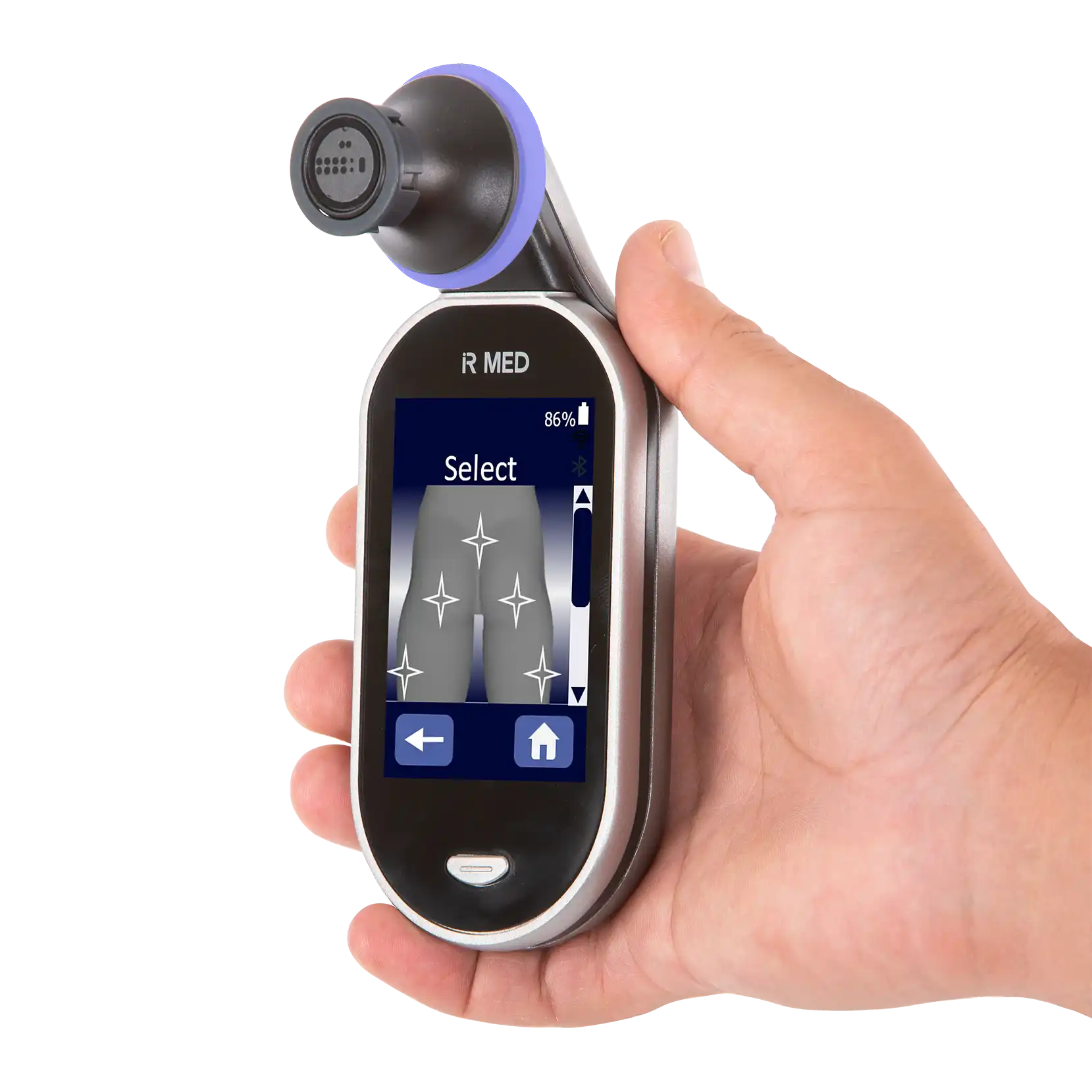
PressureSafe, IR-MED’s first product, is a handheld decision support device for assessment of pressure injuries with ~90% accuracy*, providing a novel solution to a $26B problem and driving healthcare equality for people of all skin tones

Pressure Injury - A tremendous healthcare burden
- 2.5 million patients per year develop a pressure injury
- Patient care cost per pressure injury ranges from $20,900 up to $151,700
- One of the 5 most common harms experienced by patients
- 2nd most common claim for lawsuits after wrongful death
Pressure injuries occur across the healthcare spectrum
- 10% are acute care patients
- 25% are long term acute care patients
- 12% are in nursing homes
- 12% are in rehabilitation centers

2.5 MILLION patients per year develop pressure injuries

60,000 patients die every year as a direct result of pressure injuries.

Patients with hospital acquired pressure injuries have a median excess length of stay of 4.31 days.

Patients with HAPI have higher 30-day readmission rates (22.6% vs. 17.6%)

HAPI rates are increasing. All other hospital acquired conditions are decreasing (AHRQ, 2019).

17,000 lawsuits directly related to pressure injury.
Major source of inequity in healthcare
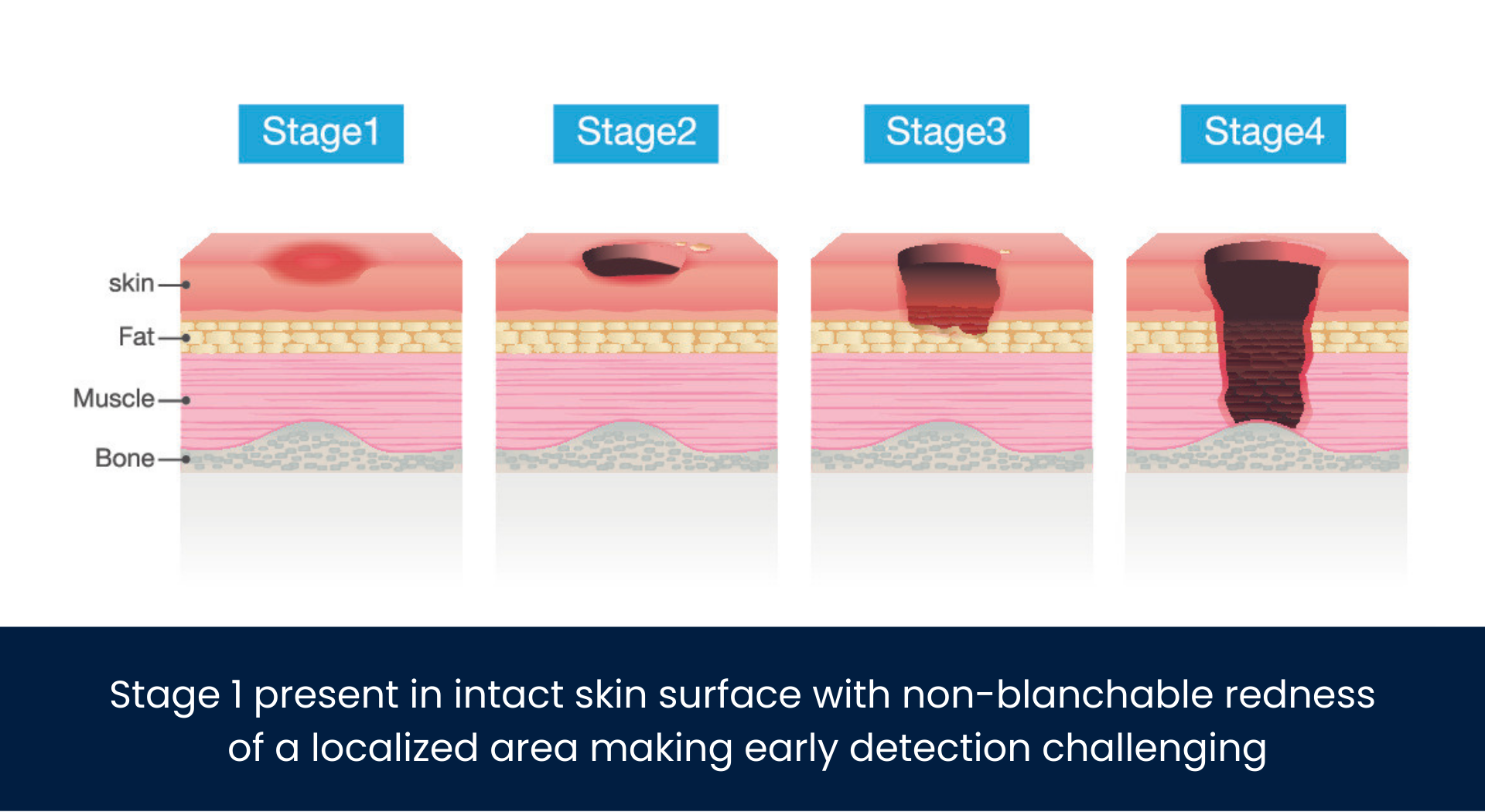
Pressure injuries are far less likely to be detected by visual inspection on patients having dark skin tones. This delay in early identification of PI and start of treatment is often devasting to the patient.
Research shows that people with dark skin tones suffer from pressure injury more than twice as much as those with lighter skin including:
- Higher pressure injury rates
- Higher risks of mortality from pressure injuries
- More severe pressure injuries
Source: NPIAP Fact Sheet 2023
Drivers for adoption of PressureSafe for assessment of Pressure Injuries
Hospitals should invest more in quality improvement and care for pressure injury to avoid higher costs.
$26.8 billion
total cost of acute care attributable to hospital-acquired pressure injuries; Medicare beneficiaries alone account for $22 billion
Reduced reimbursement related to hospital-acquired pressure injuries; Hospitals need to cover more of this financial burden.
Although hospital-acquired pressure injuries are preventable, 2.5 million people get them in acute care facilities every year
Results in extensive harm to patients – chronic wounds and 60,000 death annually
Source: “The national cost of hospital-acquired pressure injuries in the United States” International ⦁ Wouotend Journal, January 28, 2019